(Featured Image: https://stock.adobe.com/uk/images/woman-take-uterus-billboard/196513325?prev_url=detail (Licensed))
“My surgery was over in about 5 hours. Weeks later, I felt like a new person. He shared with me a video of my surgery, and for the first time, I could see the twisted mess inside me that endometriosis had made. And then I watched him remove it all. It was cathartic.”[1]

Dear Reader,
Did you know that the sufferers of Endometriosis are called as Endo-warriors? American pop singer Halsey began this movement using the term #Endowarriors to raise awareness on the social media platform of Instagram.[3]
In today’s post, I want to talk about the different ways Endometriosis can be diagnosed.
Endometriosis is typically defined by
Its histology:
Extra-uterine lesions consisting of endometrial glands, endometrial stroma, and/or hemosiderin-laden macrophages. [7]
Based on location and depth:
Lesions are further described as superficial peritoneal lesions, ovarian endometrioma, or deep endometriosis.[2,7]
Among those who ultimately receive a successful definitive diagnosis, contemporary literature describes delays from symptom onset to diagnosis ranging from 4 to 11 years.[10, 11]
Moreover, although the evidence is limited, failure of timely diagnosis and adequate management may foster disease progression and adhesion formation that may compromise fertility and increase the risk of central sensitization and chronic pelvic pain.[9,13]
Diagnosis
Anamnesis (a patient’s account of their medical history)

Listening to the patient. Carry on a detailed anamnesis languidly. This simple action gives us the best approach to the disease. She has so much to tell, to show with her face and expression. In most cases, the disease can be understood just by listening.[2]
The omnipresent symptom is pain:

There are many other pain presentations that nobody even thinks of until confronted with an endometriosis patient who, incidentally, has exactly “that type of pain.” Eguardo Rolla (2019) put forth a case of a young girl that he and his team had operated last year, who had referred right shoulder pain at menstruation. At laparoscopy, a large diaphragmatic series of blue and red lesions were excised. She was relieved after surgery. [2,6]
A similar case was encountered by Singh et al. (2017). He used MRI for the clinical diagnosis of endometriosis successfully. [6]
Pelvic Examination
Data from comparative studies suggest that findings on physical examination can identify endometriosis with high accuracy.[14,15]
Bimanual pelvic palpation:

Uterosacral ligament compromise or adhesions at the Douglas pouch➟Fixed uterine retroversion and Dyspareunia(painful sexual intercourse) [2,7]
Painful uterine mobilization is another typical sign of endometriosis.[2]
Rictus of pain cannot be avoided. It will tell you exactly where the pain is more intense, helping to clinically determine the extent of the disease. The careful and expert pelvic examination provides a lot of information at a little cost.[2]
A caveat to bimanual examination is that it may not be feasible for non−sexually active adolescents/young adults and may not identify early-stage, superficial disease.[7]
Imaging
Imaging can be a useful adjunct to clinical diagnostic measures, and transvaginal ultrasound improves accuracy when used adjunctively with symptoms, patient history, and/or physical findings.[2,7,18]
Ultrasound is particularly sensitive for detecting ovarian endometriomas and deep endometriosis. Transvaginal ultrasound approaches the sensitivity and specificity needed to replace surgery for endometrioma detection.[19]
Nonetheless, not all endometriosis will be visualized by imaging, and imaging cannot be used to rule out endometriosis.
Laparoscopy
Laparoscopy is the “gold standard” for the diagnosis of endometriosis. It certifies the presence of the disease and its extension. Utilizing tissue biopsies and their pathological analysis, the aggressiveness of the lesions can be determined. It is also the opportunity to perform the initial treatment of endometriosis.[2,7]
I would like to take an opportunity to quickly explain the stages of endometriosis:
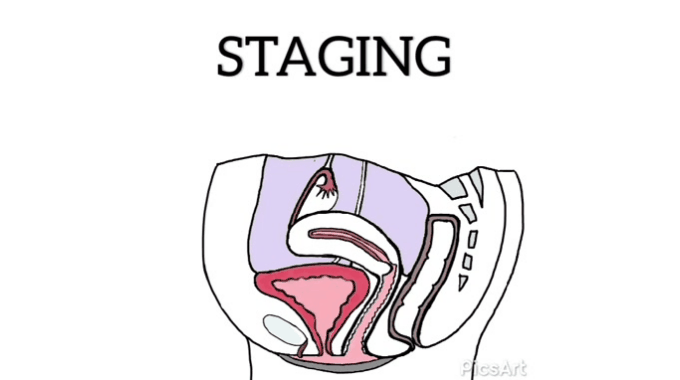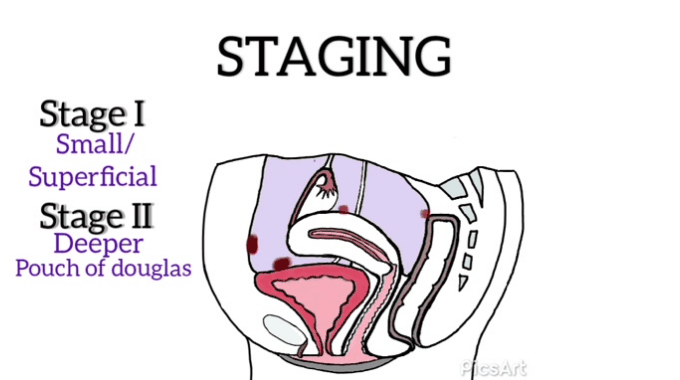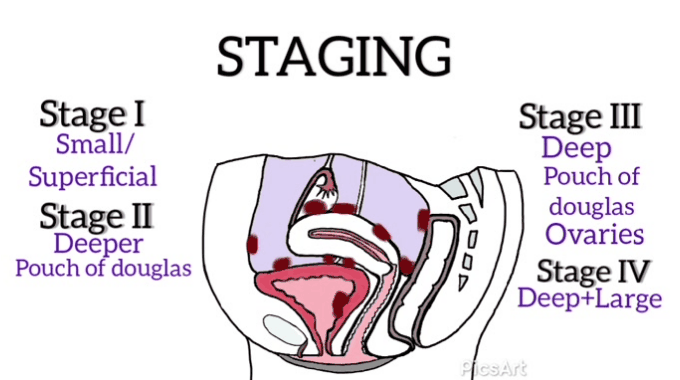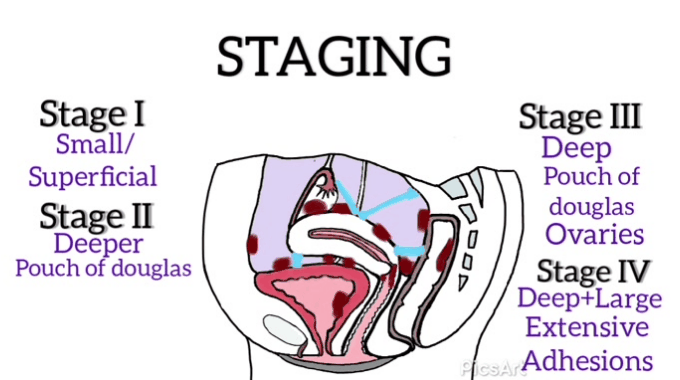
Revised American Society for Reproductive Medicine classification of endometriosis{ASRM} classifies endometriosis from Stage I (minimal) to Stage IV (severe) based on the location and size of the lesions seen during the surgical procedure (usually during exploratory surgeries).[17]
Before I end this post, I would like you to guess which month World Endometriosis Awareness is celebrated?
Until next time,
With love,
Palasha.
References:
- Flutter Health. (2017). Kristy’s Story — Flutter Health. [online] Available at: https://www.flutterhealth.com/kristys-story [Accessed 2 Jan. 2020].
- Rolla, E. (2019). Endometriosis: advances and controversies in classification, pathogenesis, diagnosis, and treatment. F1000Research, 8, F1000 Faculty Rev-529. DOI:10.12688/f1000research.14817.1
- Reimel, E. (2020). Halsey Got Real About Her Battle With Endometriosis in a Powerful Message to Fellow #Endowarriors. [online] Glamour. Available at: https://www.glamour.com/story/halsey-got-real-about-her-battle-with-endometriosis-in-a-powerful-endowarrior-instagram [Accessed 3 Jan. 2020].
- Giudice L. C. (2010). Clinical practice. Endometriosis. The New England journal of medicine, 362(25), 2389–2398. DOI:10.1056/NEJMcp1000274
- Laux-Biehlmann, A., d’ Hooghe, T., & Zollner, T. M. (2015). Menstruation pulls the trigger for inflammation and pain in endometriosis. Trends in Pharmacological Sciences, 36(5), 270–276. DOI:10.1016/j.tips.2015.03.004
- Singh, A., Das, C. J., Das, B. K., & Gupta, A. K. (2017). The utility of diffusion-weighted imaging in diagnosing subdiaphragmatic endometriosis presenting as shoulder pain. The Indian journal of radiology & imaging, 27(3), 314–317. DOI:10.4103/ijri.IJRI_86_16
- Agarwal, S., Chapron, C., Giudice, L., Laufer, M., Leyland, N., Missmer, S., Singh, S., and Taylor, H. (2019). Clinical diagnosis of endometriosis: a call to action.
-
N.P. Johnson, L. Hummelshoj, G.D. Adamson, et al. World Endometriosis Society consensus on the classification of endometriosisHum Reprod, 32 (2017), pp. 315-324
- Unger, C. A., & Laufer, M. R. (2011). Progression of Endometriosis in Non-medically Managed Adolescents: A Case Series. Journal of Pediatric and Adolescent Gynecology, 24(2), e21–e23. DOI:10.1016/j.jpag.2010.08.002
- Moradi, M., Parker, M., Sneddon, A., Lopez, V., & Ellwood, D. (2014). Impact of endometriosis on women’s lives: a qualitative study. BMC Women’s Health, 14(1). DOI:10.1186/1472-6874-14-123
- Noah, K. E., Hummelshoj, L., Webster, P., d’ Hooghe, T., de Cicco Nardone, F., de Cicco Nardone, C., … Zondervan, K. T. (2011). Impact of endometriosis on quality of life and work productivity: a multicenter study across ten countries. Fertility and Sterility, 96(2), 366–373.e8. DOI:10.1016/j.fertnstert.2011.05.090
- As-Sanie, S., Harris, R. E., Harte, S. E., Tu, F. F., Neshewat, G., & Clauw, D. J. (2013). Increased Pressure Pain Sensitivity in Women With Chronic Pelvic Pain. Obstetrics & Gynecology, 122(5), 1047–1055. DOI:10.1097/aog.0b013e3182a7e1f5
- Coxon, L., Horne, A. W., & Vincent, K. (2018). Pathophysiology of endometriosis-associated pain: A review of pelvic and central nervous system mechanisms. Best Practice & Research Clinical Obstetrics & Gynaecology. DOI:10.1016/j.bpobgyn.2018.01.014
- Bazot, M., Lafont, C., Rouzier, R., Roseau, G., Thomassin-Naggara, I., & Daraï, E. (2009). Diagnostic accuracy of physical examination, transvaginal sonography, rectal endoscopic sonography, and magnetic resonance imaging to diagnose deep infiltrating endometriosis. Fertility and Sterility, 92(6), 1825–1833. DOI:10.1016/j.fertnstert.2008.09.005
- Hudelist, G., Ballard, K., English, J., Wright, J., Banerjee, S., Mastoroudes, H., … Keckstein, J. (2011). Transvaginal sonography vs. clinical examination in the preoperative diagnosis of deep infiltrating endometriosis. Ultrasound in Obstetrics & Gynecology, 37(4), 480–487. DOI:10.1002/uog.8935
- Hudelist, G., Oberwinkler, K. H., Singer, C. F., Tuttlies, F., Rauter, G., Ritter, O., & Keckstein, J. (2009). Combination of transvaginal sonography and clinical examination for preoperative diagnosis of pelvic endometriosis. Human Reproduction, 24(5), 1018–1024. DOI:10.1093/humrep/dep013
- American Society for Reproductive. (1997). Revised American Society for Reproductive Medicine classification of endometriosis: 1996. Fertility and Sterility, 67(5), 817–821. DOI:10.1016/s0015-0282(97)81391-x
- Nnoaham, K. E., Hummelshoj, L., Kennedy, S. H., Jenkinson, C., & Zondervan, K. T. (2012). Developing symptom-based predictive models of endometriosis as a clinical screening tool: results from a multicenter study. Fertility and Sterility, 98(3), 692–701.e5. DOI:10.1016/j.fertnstert.2012.04.022
- Bossuyt, P. M., Farquhar, C., Johnson, N., & Hull, M. L. (2016). Imaging modalities for the non-invasive diagnosis of endometriosis. Cochrane Database of Systematic Reviews. DOI:10.1002/14651858.cd009591.pub2
- Fassbender, A., Burney, R. O., F. O, D., D’Hooghe, T., & Giudice, L. (2015). Update on Biomarkers for the Detection of Endometriosis. BioMed Research International, 2015, 1–14. DOI:10.1155/2015/130854
- Alimi, Y., Iwanaga, J., Loukas, M., & Tubbs, R. S. (2018). The Clinical Anatomy of Endometriosis: A Review. Cureus, 10(9), e3361. DOI:10.7759/cureus.3361
