(Featured Image: https://stock.adobe.com/images/pelvic-floor/313483255 (Licensed))

Dear Reader,
Welcome to the final blog post of this Endometriosis journey, where I want to answer the question, What constitutes in the pelvic rehabilitation session for Endometriosis patient?
Before saying anything further, I would like to state that Physiotherapy management is individualized.
Since Chronic pelvic pain in women suffering from this sinister pathology may be a manifestation of central sensitization, regardless of endometriosis-specific factors[4], Pain Management is one of the first lines of intervention.
Addressing the complexity of pain experiences physio-therapeutically means assessing and managing local tissue issues within a broader context of sensitised protective mechanisms resulting from central nervous system (CNS) sensitivity.[7,8]
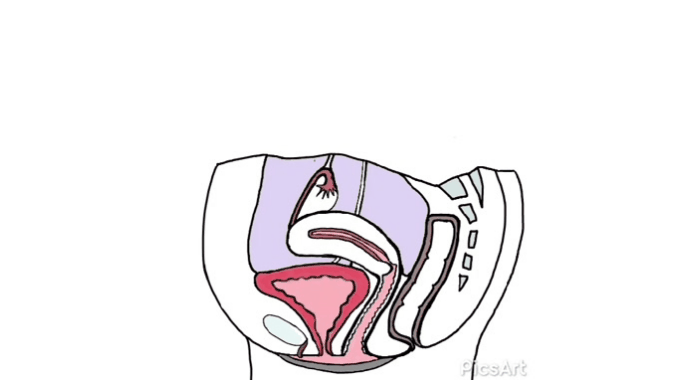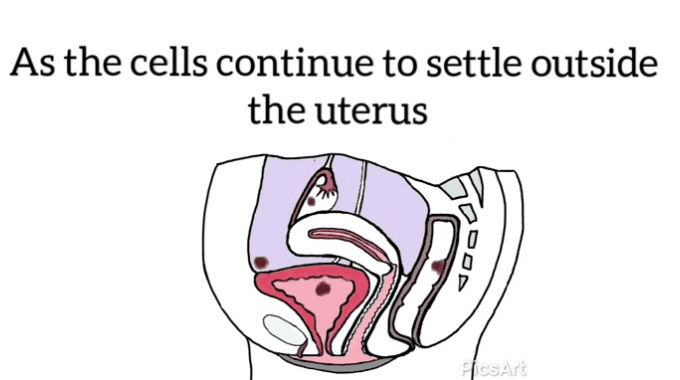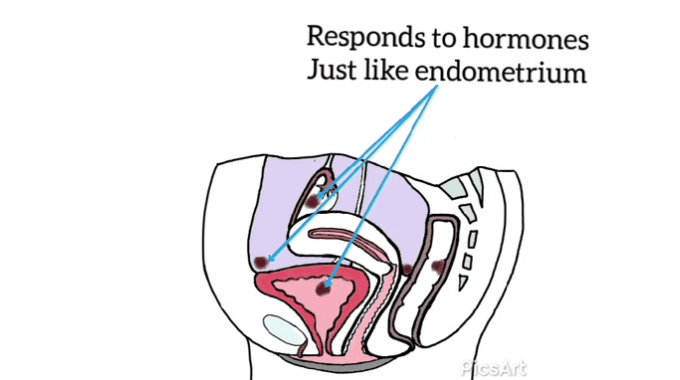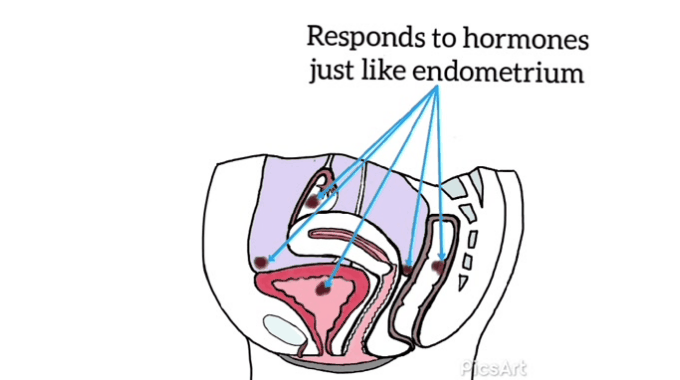
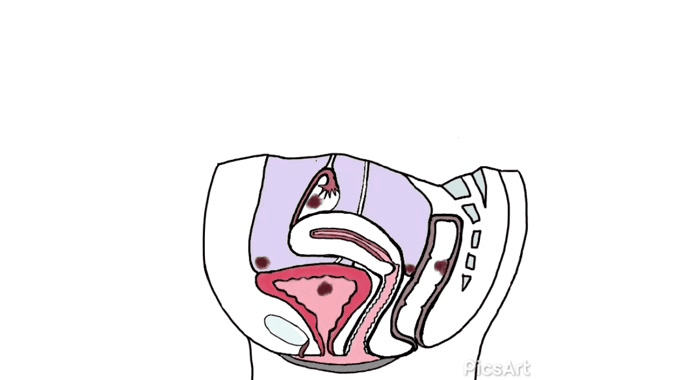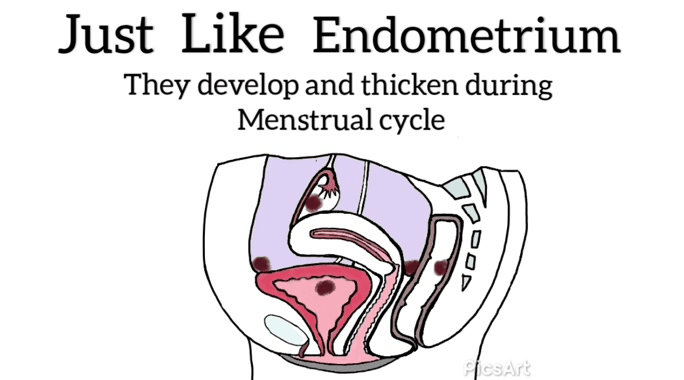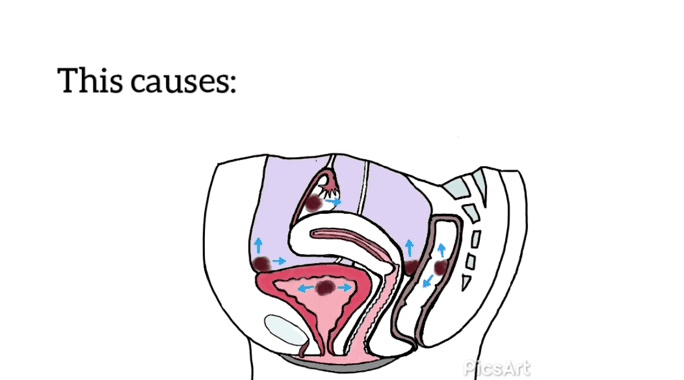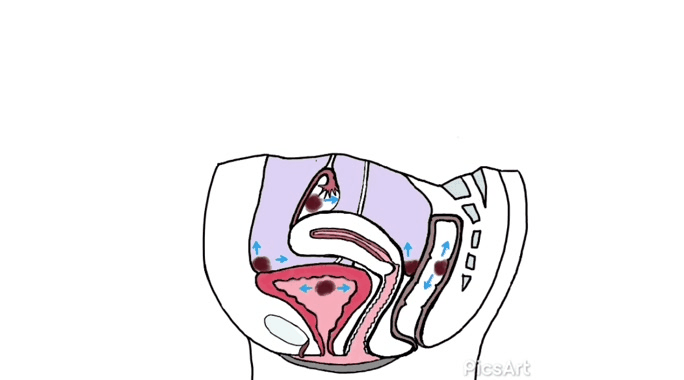
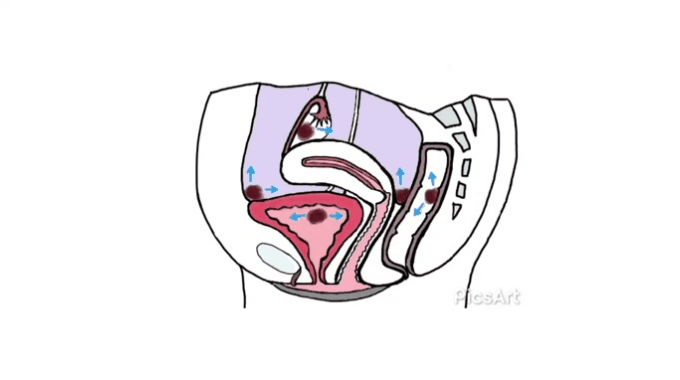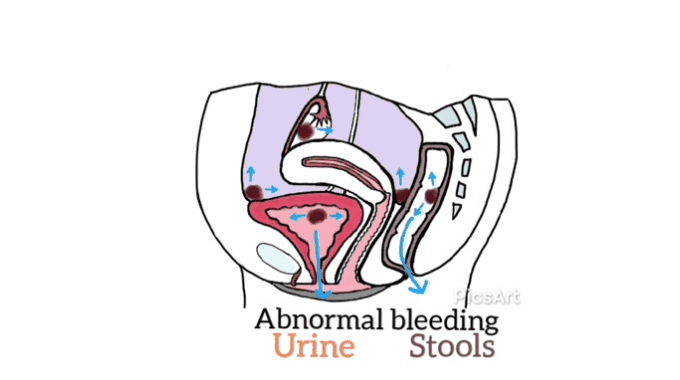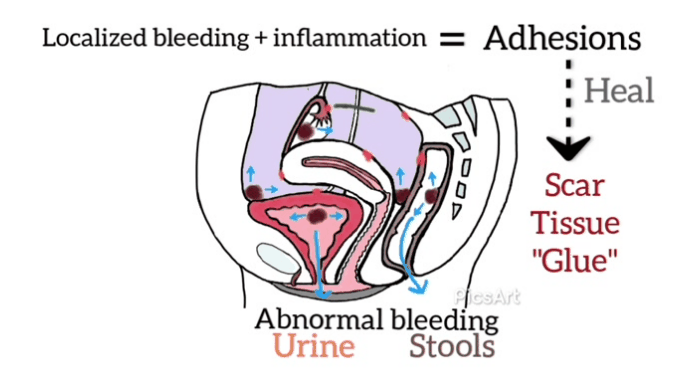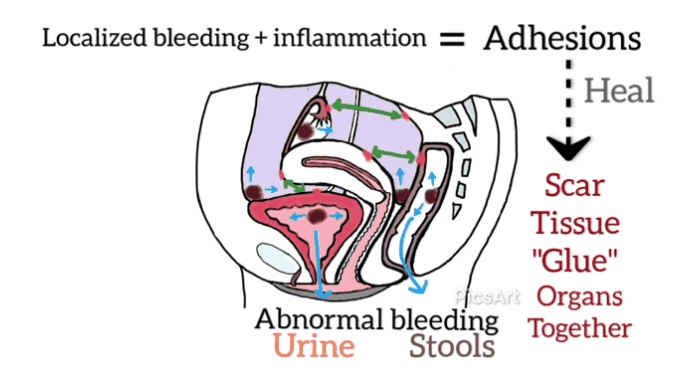
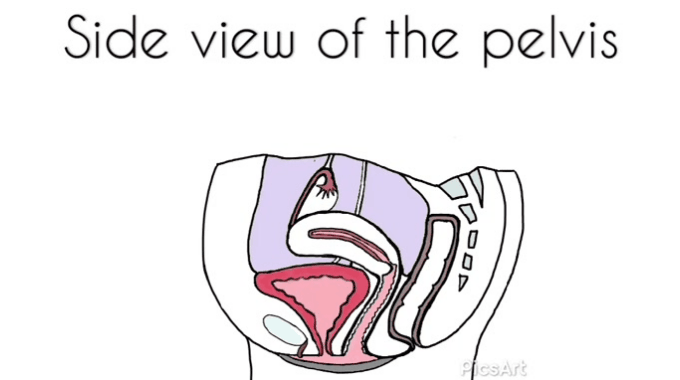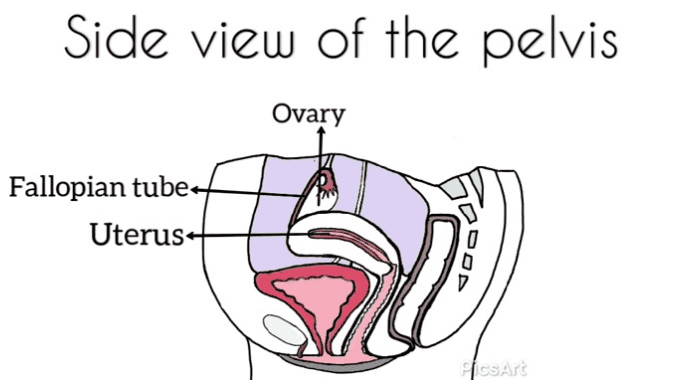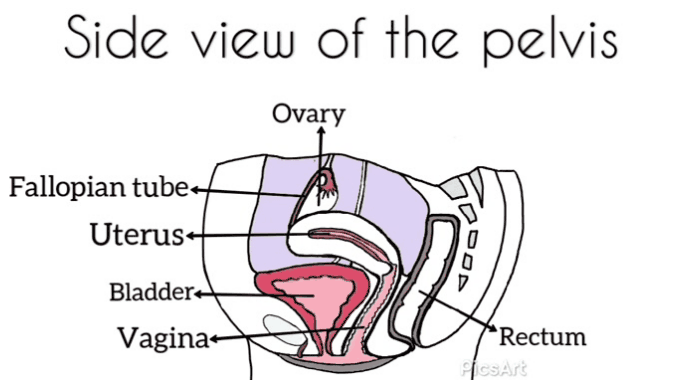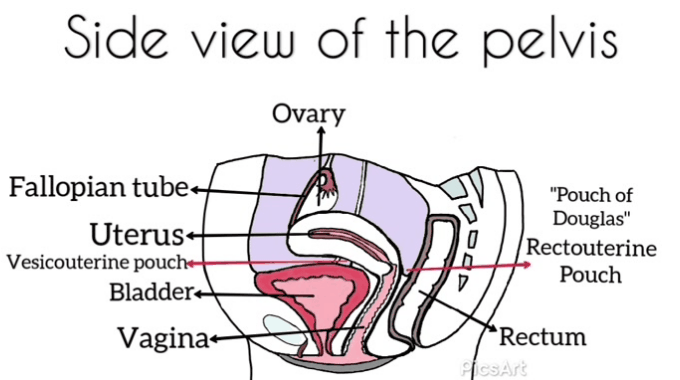
Many women have never seen images of genitalia or looked at their own vulva.[12]
Demystifying a woman’s genitalia is powerful and potentially achieved via education about anatomy, function, and vulval care. The need to normalize varied presentations as media images are very homogenized. Mirrors, pictures, and visualization may be helpful for some.[12]
Now the pelvic physiotherapy rehabilitation usually consists of posture, core stabilization (like Pilates exercises), stretching, strengthening, flexibility, coordination exercises. [15]
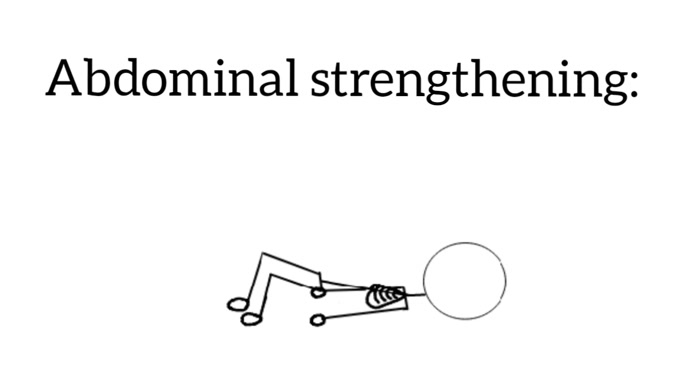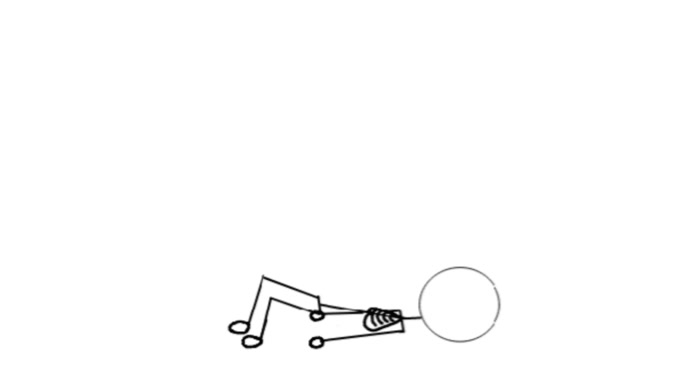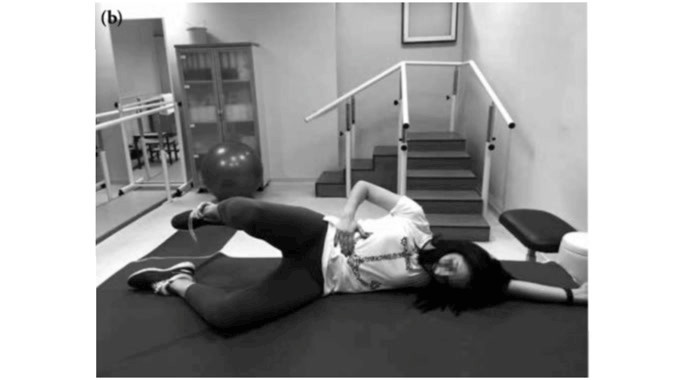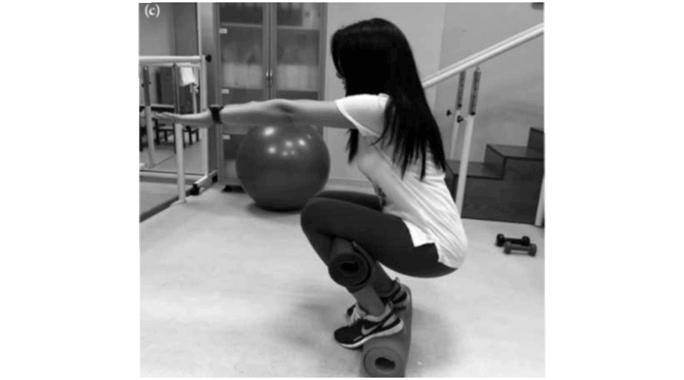
Khadiga et al. (2019) found out that Pilates was effective for treating pain and lowering blood cortisol levels in women with pelvic pain. [26] Exercises like Pilates curl, roll-up, rolling like a ball, single straight leg stretch, double leg stretch, teaser 1, Pilates pushups, shoulder bridge, single leg kick were used.

Manual therapy has the potential to reduce medication requirements in women with Chronic Pelvic Pain;[9] however, it may need delaying until some down-regulation of a sensitized central nervous system has occurred.[8]
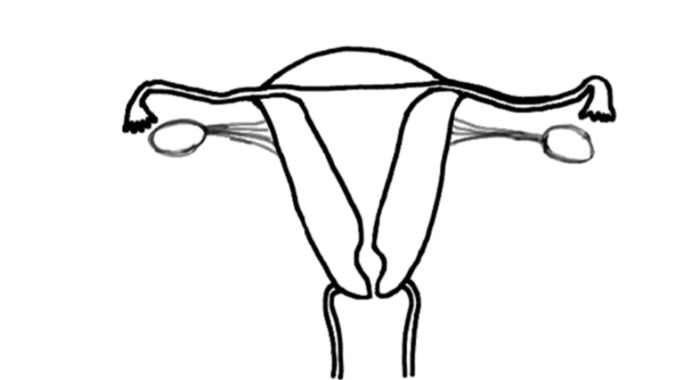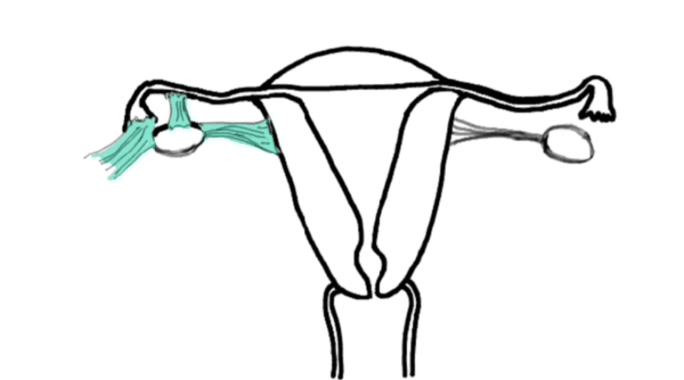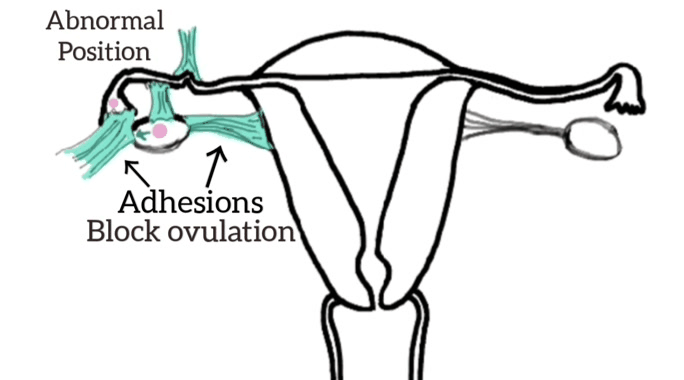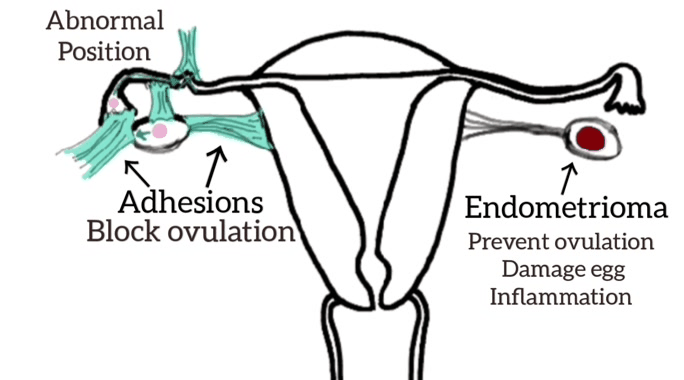
The rationale for the manual physical therapy protocol: To create micro failure of the attachments of collagen cross-links [16] since previous medical studies [17,18,19] have shown that endometriosis is frequently accompanied by adhesions.
Individualization of treatment occurred as the therapist focused on the adhesion areas, engaging the shortened soft tissues until the tissues often, indicating the release of cross-links.[19] Some of the Examples of the (Wurn’s Technique) Pelvic Manual Therapy are as follows:

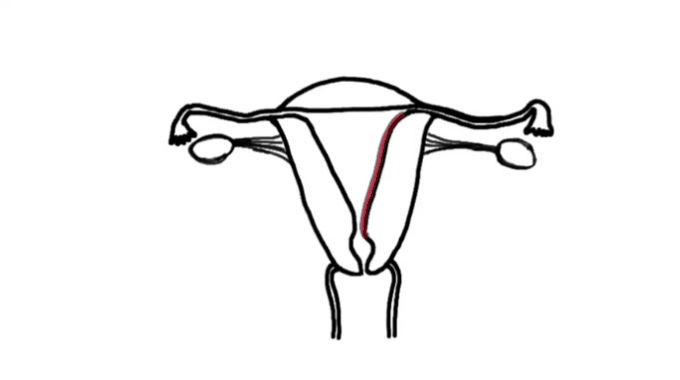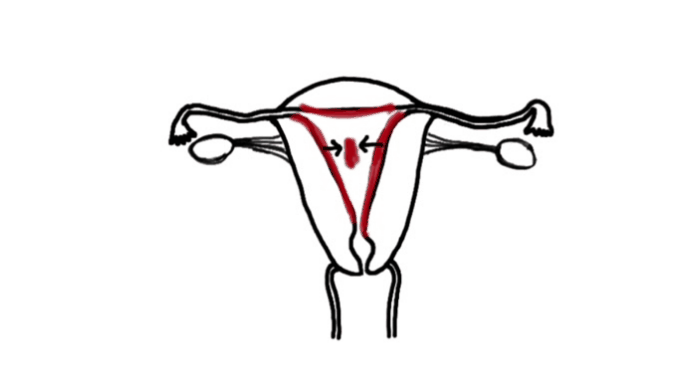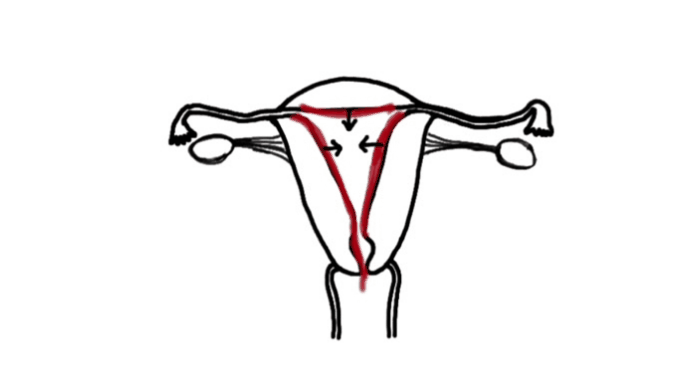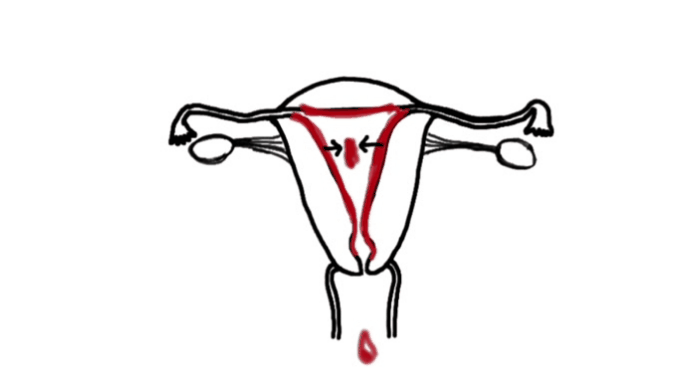
As shown in the first manual therapy example, the therapist engages the uterine fundus and sidewalls and tractions them to the left. To assist and improve the mobility of the soft tissues, the therapist may release the tension of the traction either suddenly or gradually, depending on the desired effect.[20]
In the second example, the therapist uses the leg as a lever in one of the techniques to
release adhesions from the uterine fundus.
Bi et al. (2018) found that neuromuscular electrical stimulation (NMES) useful for the treatment of endometriosis-associated pain (EAP). [25] Commonly, pelvic health physios utilize digital techniques, with or without biofeedback and intravaginal devices- To improve:
- Awareness of contraction/relaxation
- proprioception
- Confidence
- Knowledge
- Self-awareness of the vagina and Pelvic Floor Muscles
In turn, reducing hypersensitivity and stretch soft tissues.[14]
Positive physical experiences can start to modify fear-based reactions.[12]
Gentle neural mobilization techniques can be beneficial: Adverse neural tension in pudendal, ilioinguinal, iliohypogastric, femoral, or obturator nerves may contribute to pelvic pain.[13]
Pulsed high-intensity laser therapy is an effective method of pain alleviation, reducing adhesions, and improving the quality of life in women with endometriosis. [27] Its sedative action may result from several mechanisms that involve its capacity to decrease the conduction of pain impulses and to raise the rate of production of substances in human tissue that mimic the action of morphine. [28]
In addition to being a physiotherapist, I am also a yoga instructor and an Aquatic Therapist. I feel it is essential to mention the alleviating effects of them in combination with Physiotherapy bring about psychological and physical benefits to the Endometriosis sufferers [15,21,22].
It is a recipe for healing!
Yoga is an effective, time-tested method for improving overall health and managing psychosomatic and chronic degenerative disorders.[23] Yoga therapy has shown a reduction in the severity and duration of pain in women with pelvic pain. Below is the sequence used by the Saxena and his team in the targeted group:

Water exercises/ Aquatic Therapy is also another effective method added to Pelvic Physical Therapy Rehabilitation.[15] Some of the examples of the water rehabilitation: Deep and shallow water walking and running, Aerobic exercises, flexibility exercises, power, coordination, speed, and agility in addition to other specific exercises for abdominal and pelvic muscles and thighs.[15,22]
In water with lower gravity power and hydrostatic resistance as well as the lower load on joints and muscle, muscles, tendons, and ligaments can be easily strengthened. [22]
Schuch et al. (2014) found that moderate intensity, water-based exercise improved physical and psychological domains of Quality of Life, depressive symptoms, aerobic capacity, and muscular strength of women.[24]
Posture and movement should be dynamic and varied, rather than static and bracing. Exercise has benefits beyond physical fitness, including regulating sleep, improving energy, mood, and inflammation.[14]
A quick summary of the physical physiotherapy interventions:

I would like to conclude that, during my study of this complex world of Endometriosis, I found that there are very few articles dedicated to it.
That being said, I am grateful for these wonderful researchers researching in this field and I hope to join their team one day.
I owe this to the 176 million women out there.
I want to thank you, my dear Reader!
You have taken one step further in bringing out Awareness of this horrible condition. Thank you for taking the time, and I hope you enjoyed reading my blog as much as I loved writing it.
Please do share, comment, and like.
Let’s together fight in this stigma of pelvic conditions.
One awareness at a time.
Together.
With love,
Palasha.
References:
- Larbi, M., and Larbi, M. (2019). My endometriosis was so agonizing I burned myself to distract from the pain. [online] The Sun. Available at: https://www.thesun.co.uk/fabulous/9047918/endometriosis-agony-physiotherapy/ [Accessed 5 Jan. 2020].
- HE Bloomfield, A Olson, N Greer, et al. Screening pelvic examinations in asymptomatic, average-risk adult women: an evidence report for a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2014;161(1):46-53
- Buggio, L., Barbara, G., Facchin, F., Frattaruolo, M. P., Aimi, G., & Berlanda, N. (2017). Self-management and psychological-sexological interventions in patients with endometriosis: strategies, outcomes, and integration into clinical care. International Journal of Women’s Health, Volume 9, 281–293. DOI:10.2147/ijwh.s119724
- P Stratton, I Khachikyan, N Sinai, et al. Association of chronic pelvic pain and endometriosis with signs of sensitization and myofascial pain. Obstet Gynecol. 2015;125(3):719-28.
- Menstruation pulls the trigger for inflammation and pain in endometriosis. Laux-Biehlmann A, D’Hooghe T, Zollner TM. Trends Pharmacol Sci. 2015;36:270–276
- Alimi, Y., Iwanaga, J., Loukas, M., & Tubbs, R. S. (2018). The Clinical Anatomy of Endometriosis: A Review. Cureus, 10(9), e3361. DOI:10.7759/cureus.3361
- Central Sensitization, I: Pain Physiology and Evaluation for the Physical Therapist. Journal of Women’s Health Physical Therapy. 2011;35(3):103-13.
- J Nijs, B Van Houdenhove, RA Oostendorp. Recognition of central sensitization in patients with musculoskeletal pain: Application of pain neurophysiology in manual therapy practice. Man Ther. 2010;15(2):135-41.
- Anderson, RH Harvey, D Wise, et al. Chronic pelvic pain syndrome: reduction of medication use after pelvic floor physical therapy with an internal myofascial trigger point wand. Appl Psychophysiol Biofeedback. 2015;40(1):45-52.
- C Allaire, T Aksoy, M Bedaiwy, et al. An interdisciplinary approach to endometriosis-associated persistent pelvic pain. Journal of Endometriosis and Pelvic Pain Disorders. 2017;9(2):77-86.
- SJ Moore, SH Kennedy. K. The initial management of chronic pelvic pain. Green-top Guideline No. 41. Royal College of Obstetricians and Gynaecologists. 2012. Available from: www.rcog.org.uk/globalassets/documents/guidelines/gtg_41.pdf.
- S Hilton, C Vandyken. The Puzzle of Pelvic Pain—A Rehabilitation Framework for Balancing Tissue Dysfunction and Central Sensitization, I: Pain Physiology and Evaluation for the Physical Therapist. Journal of Women’s Health Physical Therapy. 2011;35(3):103-13
- C Vandyken, S Hilton. The Puzzle of Pelvic Pain. Journal of Women’s Health Physical Therapy. 2012;36(1):44-54.
- Kirkaldy, E. (2020). Physio? But I’ve got endometriosis! – O&G Magazine. [online] O&G Magazine. Available at: https://www.ogmagazine.org.au/21/2-21/physio-but-ive-got-endometriosis/#easy-footnote-bottom-56-9057 [Accessed 12 Jan. 2020].
- Vural, M. (2018). Pelvic pain rehabilitation. Turkish Journal of physical medicine and rehabilitation, 64(4), 291–299. DOI:10.5606/tftrd.2018.3616
- Threlkeld AJ. The effects of manual therapy on connective tissue. Phys Ther 1992; 72: 893-902
- Parker JD, Sinai N, Segars JH, et al. Adhesion formation after laparoscopic excision of endometriosis and lysis of adhesions. Fertil Steril 2005; 84: 1457-61.
- Luciano DE, Roy G, Luciano AA. Adhesion reformation after laparoscopic adhesiolysis: where, what type, and in whom they are most likely to recur. J Minim Invasive Gynecol 2008; 15: 44-8.
- Wurn, B. F., Wurn, L. J., Patterson, K., King, C. R., & Scharf, E. S. (2011). Decreasing Dyspareunia and Dysmenorrhea in Women with Endometriosis via a Manual Physical Therapy: Results from Two Independent Studies. Journal of Endometriosis, 3(4), 188–196. https://doi.org/10.5301/JE.2012.9088
- Wurn, L. J., Wurn, B. F., King, C. R., Roscow, A. S., Scharf, E. S., & Shuster, J. J. (2004). Increasing orgasm and decreasing dyspareunia by a manual physical therapy technique. MedGenMed: Medscape general medicine, 6(4), 47.
- Saxena, R., Gupta, M., Shankar, N., Jain, S., & Saxena, A. (2017). Effects of yogic intervention on pain scores and quality of life in females with chronic pelvic pain. International journal of yoga, 10(1), 9–15. DOI:10.4103/0973-6131.186155
- Rezvani, S., Taghian, F., & Valiani, M. (2013). The effect of aquatic exercises on primary dysmenorrhoea in nonathlete girls. Iranian journal of nursing and midwifery research, 18(5), 378–383.
- Trakroo, M., Bhavanani, A. B., Pal, G. K., Udupa, K., & Krishnamurthy, N. (2013). A comparative study of the effects of asana, pranayama, and asana-pranayama training on neurological and neuromuscular functions of Pondicherry police trainees. International journal of yoga, 6(2), 96–103. DOI:10.4103/0973-6131.113398
- Schuch, F. B., Pinto, S. S., Bagatini, N. C., Zaffari, P., Alberton, C. L., Cadore, E. L., … Kruel, L. F. M. (2014). Water-Based Exercise and Quality of Life in Women: The Role of Depressive Symptoms. Women & Health, 54(2), 161–175. DOI:10.1080/03630242.2013.870634
- Bi, X. L., & Xie, C. X. (2018). Effect of neuromuscular electrical stimulation for endometriosis-associated pain: A retrospective study. Medicine, 97(26), e11266. DOI:10.1097/MD.0000000000011266
- KHADIGA S. ABD EL-AZIZ, Ph.D., E., MOHAMAD F. ABO EL-ENEIN, M.D., A. (2019). Effect of Pilates Exercise on Primary Dysmenorrhea. The Medical Journal of Cairo University, 87(March), 1187-1192. DOI: 10.21608/mjcu.2019.53326
- Thabet, A. A. E.-M. & Alshehri, M. A. (2018). Effect of Pulsed High-Intensity Laser Therapy on Pain, Adhesions, and Quality of Life in Women Having Endometriosis: A Randomized Controlled Trial. Photomedicine and Laser Surgery, 36(7), 363–369. DOI:10.1089/pho.2017.4419
- Zati A, Valent A. Physical therapy: new technologies in rehabilitation medicine (translated to English). Edizioni Minerva Medica 2006:162–185
Featured Image: https://stock.adobe.com/images/pelvic-floor/313483255 (Licensed)